|
For instance I recently saw a tweet stating ACLR patients who couldn’t perform at least 22 single leg sit-to-stands had worse knee function post op. It can really challenge people (especially athletes) to push themselves and enhance their capacity. It can also be helpful for someone to either physically feel or visualize their deficit, instead of just hearing about it. On the flip side, sometimes specific tasks can be great for some people. Part of it has to do with how people move and perform in pain, as well as a desire to apply causation to specific variables to asymmetric and variable humans. But as evidence is past from researcher to clinician we can get tunnel vision in relation to what is important: “normal people do this, but we found that you do that” can be significant, but can also go down a rabbit hole. One issue with assessing capacity of a normal, and in-pain persons is that we can only perform analysis on one thing at a time, and we can’t extrapolate significance unless we get very particular: (good) research is designed to be able stand to scrutiny. Also in lieu of a 30-45 min treatment period perhaps 1x per week, exercise needs to be meaningful (the patient can “feel” something, has goal to achieve and they are able to work towards that in a way that ties into their understanding of their condition). One could probably drive oneself crazy if truly trying to identify and then articulate in a meaningful way that isn’t iatrogenic to the patient, the myriad of supposed dysfunction in our inherent idiosyncratic movement patterns. The mean endurance in asymptomatic men and women is roughly a 40 second hold, and 30 second hold, respectively. 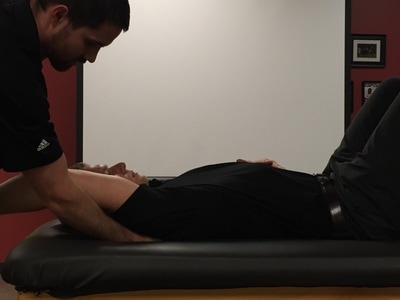
It simply looks at gross endurance, as the patient holds a chin nod in slight head elevation. The “deep neck flexor endurance” test is more of a global and less nit-picky. These altered strategies could be under conscious influence (expectation of pain) or unconscious (maladaptive habit): but the information is still only telling us what the environment is like lifting the head from supine (and not with ADL such as walking, talking, typing etc). With research that individuals with neck pain have more superficial EMG activation in their neck (and less “deep cervical flexion” action) makes sense from the view that our bodies often overcompensate in attempt to protect us, and when in pain or after injury, we move (engage) differently.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
